- Have any questions? Contact us!
- info@dr-rath-foundation.org

Worldwide Studies Show High-Dose B Vitamins Reduce Schizophrenia Symptoms
February 23, 2017
Thomas Müntzer – Violent Revolution Is Never The Answer
March 9, 2017Bisphosphonate Drugs For Osteoporosis WEAKEN Bones!

In more bad news for the pharma industry, the bisphosphonate class of drugs that are commonly used for the treatment of osteoporosis have been found to make bones weaker. In a study carried out by scientists at Imperial College in London, use of these medications was associated with the development of ‘microcracks’ in bone. Significantly, the bones of patients taking the drugs had a larger number of such cracks and less mechanical strength than those who weren’t.
The study examined bone samples from 16 osteoporosis patients aged between 60 and 90 years old. All the patients had previously suffered a broken hip, and half of them had been taking bisphosphonates. The study results revealed that the bones of people taking the drugs had 24 percent more microcracks than those not taking them. Notably, they also had 54 percent more such damage than healthy ageing bone. Describing the study outcome as “startling”, lead author Dr. Richard Abel stated: “We now urgently need larger studies to confirm this finding.”
Bisphosphonates also associated with osteonecrosis of the jaw and other serious side effects
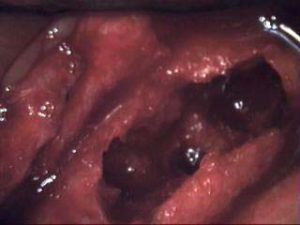
Bisphosphonate drugs have been widely associated with osteonecrosis of the jaw for over a decade now
This Imperial College study is far from being the first to identify serious problems with bisphosphonates. For over a decade now, it has been well-known that this class of drugs is associated with the development of osteonecrosis of the jaw. A severe bone disease in which the jawbone is exposed and begins to weaken and die from a lack of blood, osteonecrosis of the jaw has become widely recognized as a side effect of bisphosphonate treatment. The consequences can be so severe that, in some cases, patients need reconstructive surgery.
Other known adverse effects of bisphosphonates include gastrointestinal problems, fever, severe musculoskeletal pain, low calcium levels, cancer of the esophagus, and atrial fibrillation (a type of irregular heartbeat).
Worryingly, even if patients stop taking these drugs they can remain in their bones for years afterwards.
The Cellular Medicine approach to osteoporosis
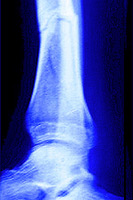
Significant healing seen at 10 weeks with miconutrients
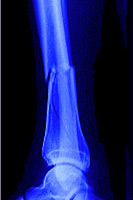
Broken bone
Dr. Rath’s groundbreaking Cellular Medicine concept describes how the primary cause of today’s most common chronic diseases is a long-term deficiency of vitamins, minerals, amino acids, and other specific micronutrients. In the case of osteoporosis, this deficiency results in the bones becoming weak and brittle, with a consequent risk of fracture. Under the Cellular Medicine approach, the most effective preventive and therapeutic responses to osteoporosis are therefore based upon an optimum daily intake of micronutrients. Numerous scientific studies now exist which demonstrate the safety and efficacy of nutritional interventions in controlling this disease.
While many people seem to believe vitamin D and calcium are the only nutrients needed for healthy bones and repairing fractures, this mistaken assumption overlooks the fact that the framework of the bone on which calcium and other minerals are deposited is made of a protein – collagen. Without healthy collagen, bone cannot form or function properly.
Healthy bone formation therefore depends not only on sufficient amounts of calcium and vitamin D, but more importantly on a proper supply of vitamin C, the amino acids lysine and proline, and other collagen-supporting micronutrients. For patients suffering from bone fractures, including these critical nutrients in a synergistically designed supplement program can significantly reduce healing time and improve general feelings of wellbeing.
As with other chronic diseases, it can accordingly be seen that only nutritional and Cellular Medicine approaches provide the long-term answer to successfully addressing the primary cause of osteoporosis. The larger the number of doctors and patients we can communicate this important information to, the sooner this degenerative bone disease can become a thing of the past.



