- Have any questions? Contact us!
- info@dr-rath-foundation.org

Health Protective Effects of Phytonutrients: Green Tea Extract
October 4, 2017
Our Study Proves That Heart Disease Is Linked To Vitamin C Deficiency
October 4, 2017The Benefits of Micronutrients in Heart Failure
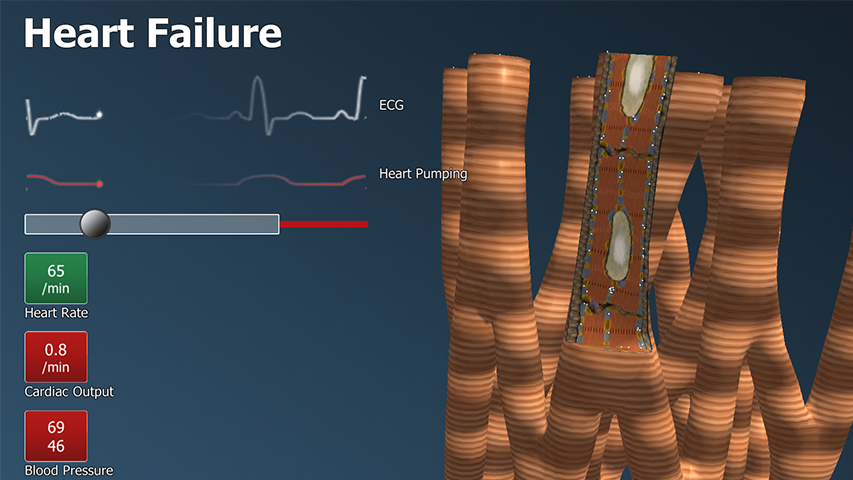
The correlation between micronutrient deficiency in the diet, lack of energy in the heart muscle and reduced heart pumping function (heart failure) can be examined interactively and in detail on the BodyXQ website: www.bodyxq.org
Heart failure is a serious health condition where the heart is unable to pump enough oxygenated blood to other parts of the body. According to the US Centers for Disease Control and Prevention (CDC), about 5.1 million people in the United States are affected by heart failure with around 40-50% of them dying within one year of diagnosis. The economic impact of heart failure is huge as the cost of treating Americans for heart failure costs an average of about $32 billion annually, including absences from work. Worldwide, approximately 23 million people suffer from heart failure.
Heart failure commonly follows the development of another cardiovascular condition such as atherosclerosis, high blood pressure, diabetes, heart irregularities (arrhythmias), heart valve disorders or cardiomyopathy. Obesity, smoking, living a sedentary lifestyle or having a family history of heart disease further contribute to the development of heart failure. Common symptoms of heart failure include fatigue, shortness of breath, dizziness, a long standing cough and wheezing, as well as swelling of the ankles, legs and abdomen.
The human heart is a muscle that requires tremendous amounts of energy, in the form of ATP (adenosine triphosphate), in order to function properly. This energy is needed to support the heart’s regular beating (it beats 100,000 times per day) and to recycle blood (5 liters are propelled though the body every minute). Whilst a lack of this vital energy is the most important reason for heart failure, conventional treatment approaches ignore this fact. Instead, the conventional treatment of heart failure usually involves medications such as diuretics and beta-blockers that offer only symptomatic relief by reducing the swelling of the heart muscle or increasing the ease of breathing. Diuretics are used for the primary treatment of heart failure in order to reduce edema by removing water accumulated in the tissues. However, diuretics also wash out critical watersoluble vitamins such as vitamins C and B1, as well as minerals such as Potassium, Calcium, Magnesium and Zinc etc. These micronutrients are essential to support proper contraction and relaxation of the heart muscle cells. Beta-blockers strip the body of Coenzyme Q10 (CoQ10), a nutrient which is essential for the generation of ATP in cellular mitochondria. Digoxin depletes Magnesium and B vitamins, which are essential for optimum bioenergy production in cells. It is proven that deficiency of the nutrients CoQ10, vitamin C and vitamin B1 increases the risk of heart failure.
We conducted a pilot clinical trial in heart failure patients aged between 41 and 68 years old1. These patients took a specific combination of micronutrients for six months. The results showed remarkably improved cardiac pumping action (symptomatic improvement) and therefore an improved quality of life in the participants. At the beginning of the study, 70 percent of patients were suffering from an extensive impairment of cardiovascular health and their daily activities. Thirty percent of patients reported a moderate limitation of their daily physical activities. At the end of the study, 80 percent of the patients reported improvement in their health condition by one or more grades on the New York Heart Association scale. After six months, half of the patients could lead normal lives again without any discomfort or associated symptoms.
Other clinical studies have repeated and confirmed similar findings, thus emphasizing the importance of micronutrient supplementation2. Conventional heart failure medicines act only to deplete the essential micronutrients required for optimum heart function. Therefore, micronutrient supplementation is the only effective way to provide bio-energy for the optimum functioning of heart muscle cells.
Ref:
1 Cellular Health Communications Vol 1, No. 1, 2001
2 Witte KK, et al., Eur Heart J. 2005 Nov; 26(21):2238-44



